
The liver is the largest internal organ in humans, weighing approx. 1.5 kg.1 As the metabolic hub of the body, it is closely involved in the production, storage and utilisation of fats, sugars and proteins, filtering pollutants, alcohol and other toxins, producing bile acids and cholesterol, which are important for the digestion of fats, and producing a number of hormones.1,2
An inflammation of the liver is known technically as “hepatitis”, derived from the Greek “hepar” = liver. The suffix “-itis” refers to an inflammation. Triggers include, for example, alcohol abuse, dysfunctions of the immune system (so-called autoimmune hepatitis), inflammation of the bile ducts, excessive use of drugs that damage the liver or fatty degeneration of the liver, often in combination with obesity and diabetes.3
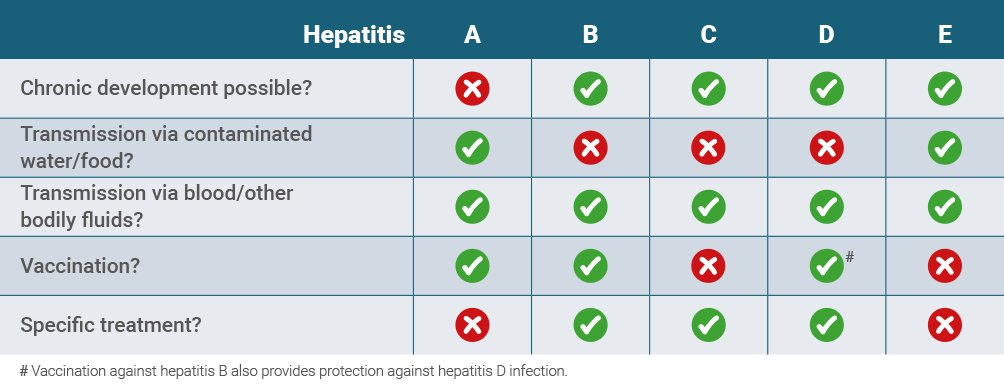
Certain viruses can also cause inflammation of the liver. There are currently five different types of hepatitis known, they are labelled with the letters A to E.3
Hepatitis B, C and D are of particular medical importance. They may become chronic and then lead to serious secondary diseases such as cirrhosis of the liver or liver cancer.3
You will find an overview of the different types of hepatitis in the following table.4-7
Despite all its functions, the liver is unable to do one thing – cause pain. Inflammation of the liver can therefore often go completely undetected or with symptoms that are very unspecific and are not often attributed to liver disease by those affected.3 That is what is so dangerous. Those suffering from fatigue, a feeling of pressure in the right upper abdomen, joint pain, itching or even dark urine over an extended period of time should consult a doctor to be on the safe side.3,8 Only the most severe cases of the disease are characterised by yellowing of the skin and eyes (jaundice), intense pain in the upper abdomen, vomiting and extreme fatigue.3 The doctor can use a blood sample to specifically check the liver parameters in a laboratory analysis and if these liver parameters are elevated, a check must be made for a possible viral infection.3,9
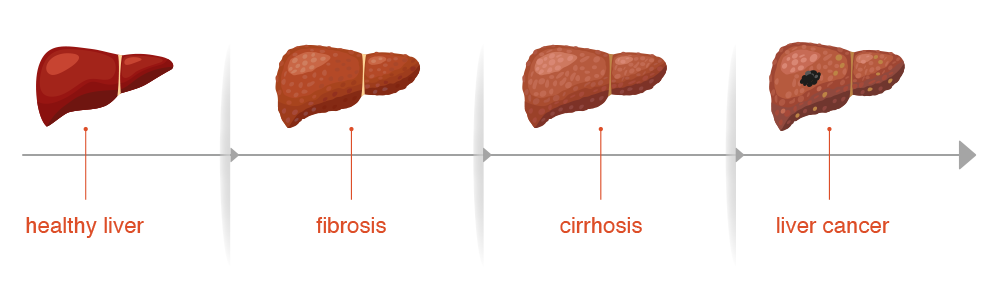
First of all, the liver tries to repair the damage itself: it produces new, healthy cells. In cases of permanent, chronic inflammation, it is often no longer able to achieve this and the liver cells are replaced by scarred connective tissue – a condition known as fibrosis develops. The liver can still carry out its functions if there is fibrosis. Progressive scarring, however, eventually leads to cirrhosis.
The liver can no longer fully perform its metabolic and detoxification functions at this stage. Fibrosis developing into cirrhosis can be a gradual process that can take many years, possibly even decades.10
Serious complications of cirrhosis include the accumulation of fluid in the tissues (oedema), in the abdomen (ascites), an increased tendency to bleed, varicose veins in the oesophagus or diseases of the brain.10
In principle, every patient with liver cirrhosis has an increased risk of liver cell cancer. Up to 8% of all patients with liver cirrhosis develop liver cell carcinoma.
Depending on the cause, the risk of developing:
• chronic hepatitis B is 2%
• chronic hepatitis C is 3-8%11

If you want to find out more about hepatitis B, you can find a lot of useful information here.

What actually is hepatitis C? Here you will find useful explanations.

Find out more about hepatitis D! What makes it different from hepatitis B? And how can you protect yourself?